Eczema and Dermatitis are both general terms to describe skin irritation or inflammation of the skin. Both terms are used to describe various types of skin conditions, including rashes and red-colored dry patches on the skin. Most of the time, both words are used interchangeably. However, there are specific types of skin conditions that are known just by one of the names. For instance, “atopic dermatitis” can be used interchangeably with “eczema,” but “contact dermatitis” cannot be used in place of “eczema.” Eczema and dermatitis are not contagious, but they can make you feel self-conscious and uncomfortable.
Eczema and dermatitis have many types and you can have more than one type at one time. Both eczema and dermatitis cause itching and redness, but some types cause peeling and blistering. The following are the types of eczema and dermatitis.
Atopic dermatitis or eczema is a skin condition characterized by red, itchy, and dry skin. Although the condition is common in children, it can occur on people of all ages. It is a chronic (long-lasting condition) and usually flares periodically. Normal and healthy skin retains moisture and protects you from allergens, bacteria, and irritants. Atopic dermatitis is related to a gene variation that makes the skin unable to provide protection, allowing your skin to be affected by allergens, irritants, and other environmental factors. For some children, atopic dermatitis can also be caused by food allergies. The symptoms can vary widely from one person to another, the symptoms include:
- Itching that can be severe, particularly at night
- Dry skin
- Sensitive swollen skin as a result of scratching
- Thickened, scaly, and cracked skin
- Red or brownish-grey colored patches on the feet, hands, ankles, neck, waist, upper chest, eyelids, inside the bend of elbows, and knees. In infants, the patches can be found on the face and the scalp.
- Small and raised bumps that can crust over or leak fluid when scratched.
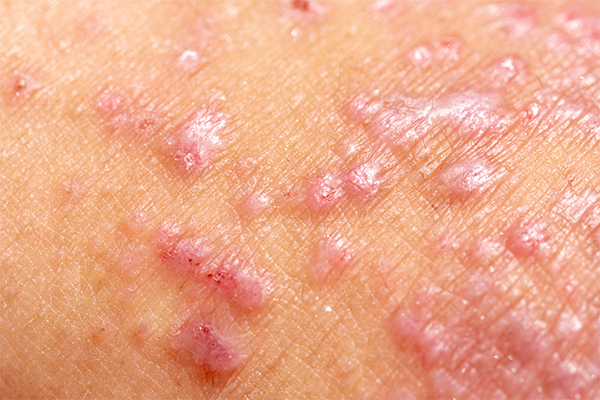
Sometimes, atopic dermatitis may also be accompanied by hay fever or asthma. If you or your child has a skin infection, feel very uncomfortable because the condition is affecting daily activities and sleep, or if the symptoms don’t improve after home remedies, it is advisable for you to go see a doctor.
Contact dermatitis is an itchy and red rash caused by direct contact with a substance or an allergic reaction to that substance. These substances can include cosmetics, fragrances, soaps, plants, and jewelry. Contact dermatitis usually occurs in areas of your body that have been exposed to the substances that cause your skin to react. The rash can develop after a few minutes to hours of direct exposure and may last between two and four weeks. The symptoms of contact dermatitis include:
- Itching, sometimes severe
- Red rash
- Dry, scaly, and cracked skin
- Blisters and bumps, which may crust or ooze
- Burning and swelling
You will need to see a doctor if the rash is sudden, severe, painful, or if it doesn’t get better in three weeks, affect your face or genitals, and distracts you from your daily activities and sleep. You may also need to get immediate medical care if your lungs, nasal passages, or eyes are painful and inflamed. To treat contact dermatitis, you need to know the cause of the reaction so you can completely avoid it.
Seborrheic dermatitis is a very common skin disease that usually affects the scalp and causes red skin, scaly patches, and dandruff. It can also affect areas on your body that are oily, including the sides of your nose, face, eyebrows, eyelids, ears, and chest. The condition is also known as seborrheic eczema, seborrheic psoriasis, or dandruff. The exact cause of this condition is unknown. However, it may be related to an irregular response of your immune system and a fungus (yeast) in the oil secretion on your skin. Some risk factors can increase your risk of developing seborrheic dermatitis, such as:
- Recovery from some medical conditions, including a heart attack
- Psychiatric and neurologic conditions, such as depression and Parkinson’s disease
- The weakened immune system, usually in people with HIV/AIDS, organ transplant recipients, alcoholic pancreatitis, and certain cancers
- Some medications.
- The symptoms of seborrheic dermatitis can be more severe if you are stressed and they tend to flare in dry and cold seasons. The symptoms are:
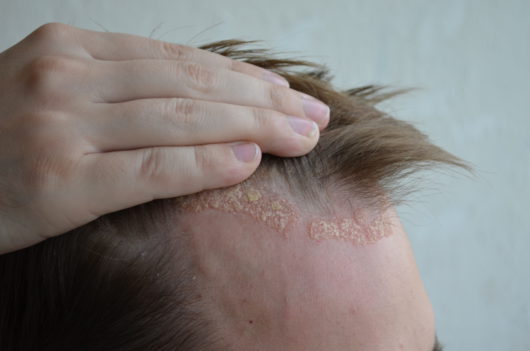
- Skin flakes (dandruff) on your hair, scalp, eyebrows, mustache, or beard
- Red skin
- Itching
- Flaky white or yellow scales that cover patches of greasy skin or crust on the face, sides of the nose, scalp, ears, eyebrows, eyelids, armpits, groin area, chest, or under the breasts.
There are numerous other types of eczema and dermatitis, including follicular eczema, stasis dermatitis, dyshidrotic eczema, nummular eczema, hand eczema, dermatitis herpetiformis, asteatotic eczema, discoid eczema, neurodermatitis, and pompholyx eczema. To find out which type of eczema and dermatitis you have, you need to see your doctor so your doctor can diagnose and provide a plan for treatment. Talking about your symptoms and examining your skin is the first step your doctor takes to diagnose your condition. Your doctor may also perform patch testing on your skin and biopsy.
Because the symptoms of eczema are virtually the same, they’re also treated fairly similarly. Some types of eczema and dermatitis can be treated with lifestyle changes and home remedies. This includes:
- Apply a moisturizer to your skin regularly.
- Use over-the-counter hydrocortisone cream or an oral antihistamine to temporarily relieve itching and redness.
- Apply a cool wet cloth to help soothe your skin.
- Take a warm bath. You can sprinkle baking soda or colloidal oatmeal to your bathwater, soak your skin for around 5 to 10 minutes, pat dry and apply moisturizer while your skin is damp.
- Use medicated shampoos. If you have dandruff, you can use shampoos that contain zinc pyrithione, ketoconazole, coal tar, or selenium sulfide.
- Avoid rubbing or scratching the itchy areas.
- Use mild and unscented laundry detergent
- Wear smooth-textured cotton clothing to avoid irritating the affected area.
- Avoid your irritant or allergen.
- Manage your stress because emotional stressors can cause some dermatitis to flare up.
In addition, your doctor may also suggest you do the following treatment.
- Use certain creams or ointments that affect your immune system.
- Take oral corticosteroids (pills) or injectable dupilumab.
- Expose the affected area to natural or artificial light (phototherapy).
- Apply corticosteroid creams, ointments, or gels to the affected skin.

